Heel Bone Spurs
By Dr. Dina Elsalamony MD, MScPH
It shouldn’t hurt to get on your feet in the morning or walk throughout the day. If you notice a sharp, stabbing sensation in your heel with each step you take, you may be suffering from heel spurs.
What Is A Heel Spur?
A heel spur is the excess build-up of the calcium deposits over a long time on the calcaneal bone, commonly known as the heel bone, leading to a bony outgrowth formation. The bony outgrowth can appear as hooked, pointy, or shelf-shaped, and differs in size from one individual to another, however, it can grow up to half an inch in length. Heel spurs can be linked to excessive strain, abnormal biomechanics, or less commonly, underlying health conditions.
A heel spur can either be a plantar heel spur, which is the most common and exists on the bottom of the feet, or a posterior heel spur that forms on the back of the heel.
Calcaneal spurs are a common condition, a study has reported that on average, 32% of people have plantar heel spurs, while about 13% experience posterior heel spurs. The highest incidence of 41.8% was detected in those over the age of 70 years old, and females were reported to have a higher incidence of developing posterior heel spurs than males. (1)
Despite being a fairly common condition, not everyone will experience pain as a result of growing heel spurs a large number of the cases are discovered accidentally during x-ray tests that were ordered for other feet issues. However, when the pain is felt due to heel spurs, it can be intense and interfere with everyday normal activities.
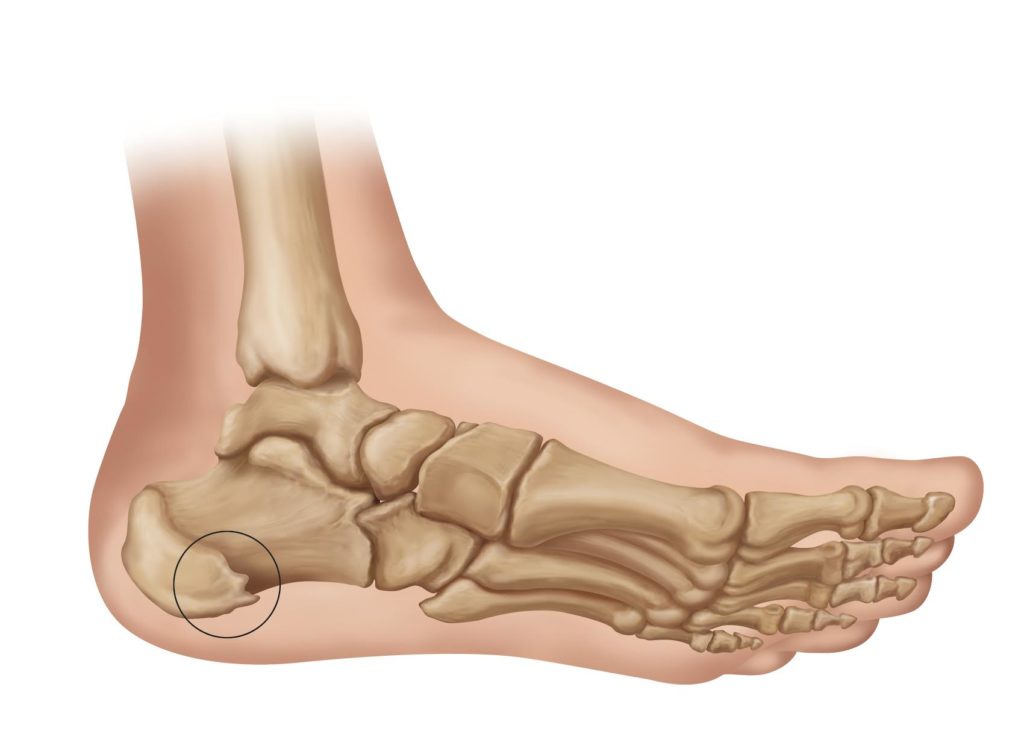
What are the types of heel spurs?
Heel bone spurs are categorized, based on their location, into the following:
Plantar calcaneal spur:
Plantar calcaneal spurs are the most common type and are also known as heel spur syndrome. It involves the formation of the bony projection in the plantar area (the bottom of the heel), they typically grow where the calcaneal bone connects to the plantar fascia, which is a collagenous fibrous tissue band stretching across the bottom of the foot. Hence, this type of heel spurs is commonly mistaken with plantar fasciitis, which is a degenerative condition of the plantar fascia, and despite it coexisting with plantar fasciitis in a large number of cases, these 2 conditions are different and distinct from each other.
Posterior calcaneal spur:
Posterior calcaneal spurs form on the back of the heel and often are associated with a condition called insertional Achilles tendonitis, which involves inflammation of the Achilles tendon. The bone spur in this case grows gradually surrounding the part of the tendon where it is inserted into the heel bone.
What causes heel spurs?
The exact cause of heel spurs has been difficult to determine. Initially, it was thought that plantar heel spurs developed as a result of repetitive traction of the plantar fascia’s insertion into the calcaneus bone, leading to inflammation and subsequent bone formation. (2) However, this theory was challenged by other scientists proposing that traction is the cause of the posterior/ Achilles spurs and not the plantar ones, as when traction happens around the Achilles tendon, posterior spurs always form within the tendon, while in the case of plantar spurs, almost half of them are not formed within the plantar fascia, which suggests other reasons are involved. One of these reasons is vertical compression since the bony protrusion is often vertically oriented and that plantar spurs are associated much more with excess weight or long periods of standing, while posterior spurs are more common with sustained activities. (3)
Some believe that the natural process of aging also has a hand in developing heel spurs, in addition to the higher tendency for older individuals to have calcium deposits forming excess small bony parts, aging itself can cause stiffness of the heel pad and decrease its ability to soften the force endured during impacts, leading to repetitive stress and microtrauma which eventually contribute to the bony development. (4)
Finally, genetics may also well play a role in developing heel spurs; some people have a genetic predisposition for new bone formation responding to a certain level of mechanical stressors, which explains why other people don’t develop spurs even when subjected to the same or greater level of mechanical stress. (5)
What Are the Risk Factors of Heel Spurs?
- Foot position and structural issues: the structure of the feet and how this affects where your feet land when touching the ground, and the dynamics of your gait, play a role in developing heel spurs. For example, when your feet roll towards the inside when you walk, transferring your body’s weight to the inner edge instead of the ball of the foot, this is called overpronation of the feet and has been significantly associated with the formation of plantar heel spurs. Having flat or high arched feet have also been linked to the development of heel spurs.
- Obesity: a study found that 82% of those with plantar heel spurs are either overweight or obese (6), another study reported that those with plantar heel spurs are about 7 times more likely to be obese when compared to those who don’t have the condition. (4)
- Older age: the incidence of heel spurs increases greatly with age, on average about 55% of those above 62 years old may have some form of heel spurs, it was also found that 98.4% of those who have plantar heel spurs are above the age of 40. Degenerative changes and alteration of the gait patterns with old age are thought to contribute to this high prevalence.
- Rheumatoid disorders: plantar heel spurs are commonly found in any rheumatology-related disorder. Those with plantar heel spurs when compared to those who don’t, were found to be 3 to 10 times more likely to have one area in their body that exhibits osteoarthritis.
- Being female: studies have found that generally in older age the incidence of developing heel spurs is similar between females and males, while in younger populations, up to 49 years of age, females were found to have a much higher incidence than males, which was theorized to be as a result of wearing high heels that can alter the normal feet biomechanics. (7)
- Plantar fasciitis: there is a strong statistical association between having plantar fasciitis and developing heel spurs; in fact, plantar heel spurs are present in 45% to 85% of those who have plantar fasciitis, this is thought to be due to both of these conditions sharing similar risk factors, and that the impact of plantar fasciitis on the feet can and indirectly contribute to the formation of plantar heel spurs.
- Certain physical activities that increase the load and impact on the feet such as running, jogging, and jumping.
- Inappropriate footwear: poorly fitted shoes can change how a person walks and puts pressure on more areas than others. Old worn-out shoes, high heels, or shoes without enough cushioning can all negatively affect the feet due to the lack of shock absorption or padding, which reduces the impact of high vertical loading on the feet.
- Diabetes: although it is not fully established as a risk factor for developing heel spurs, some studies have found links between the two. For example, a study has reported that those who have plantar heel spurs are 4 times more likely to also have diabetes. (6)
- Trauma to the heel can also contribute to the formation of heel spurs.
What are the symptoms of heel spurs?
How do you know if you have a heel spur? Actually, in a large number of cases, heel spurs can be asymptomatic, however, when symptoms are present, heel spurs can be very painful and a cause of discomfort. Heel spur pain is often due to the contact of the spur with the surrounding tissues, leading to friction and inflammation.
The pain associated with heel spurs can be acute, intermittent, or chronic, and it is exacerbated during high-impact or weight-bearing activities such as walking, jogging, or running. It is usually described as stabbing or sharp pain that occurs particularly when taking the first steps in the morning and may continue in a duller form throughout the rest of the day. Swelling and skin warmth around the heel may also happen, and tenderness of a specific area can be felt when pressed against with hands or when the feet come in direct contact with hard surfaces. In some cases, the small bony protrusion can be felt or even seen under the heel. If your symptoms resemble those mentioned, then you may have a heel spur, however, an accurate diagnosis by a physician is very important as other heel conditions may also share some of these symptoms.
How are heel spurs diagnosed?
To get a confirmed diagnosis with heel spurs or just get to the bottom of addressing the cause and management of your symptoms, you should book an appointment with your general practitioner for an initial consultation, or book directly with a specialist such as a podiatrist or an orthopedic doctor. Your doctor will ask you about the history of your pain, your medical and occupational history so they will be able to determine if you have any risk factors. Your doctor then will proceed to examine your feet, checking for tenderness, redness, or swelling, also checking for any deformities or structural issues, and ask you to walk to observe your gait or stand on one foot at a time to see how you carry your body weight.
Your doctor might be able to feel or see the bony protrusion, however, it is not common for heel spurs to be visible, hence, he/she will probably then ask for an X-ray to confirm the heel spur diagnosis and ensure that no other issue is the cause behind your symptoms.
How are heel spurs treated?
Treatment for heel spurs is categorized into the following:
Conservative heel spur treatments include:
Rest: this is vital in the management and treatment of the symptoms of both heel spurs and plantar fasciitis if coexist. As we mentioned earlier, vertical weight compression is thought to be the main cause behind developing heel spurs, so resting and lifting the weight of your body from your feet can help to stop the pain and assist in faster recovery, as it will allow the natural process of healing to take place without more activities that can cause further damage. If it is not possible for you to completely rest, then activity modification is required, for example, try to use transportation instead of walking, stop any high-impact exercise, and exchange that with seated exercises. If your job requires a long period of standing, make sure to wear appropriate cushioned shoes while taking regular breaks to sit down.
Icing: cold compressions for 15 minutes can help relieve the pain and reduce the symptoms of inflammation. You can apply the ice by submerging your feet in an ice bath or using an ice pack. Alternatively, you can try Heel That Pain Ice Therapy Slippers, which allow you to strap them into your feet, so you get full coverage while being secured in place. Heel That Pain slippers ensure the entire bottom surface of your feet is properly iced, reducing pain, tenderness, and swelling.
Over-the-counter medications: OTC medications can help you manage the pain, particularly non-steroidal anti-inflammatory drugs such as Ibuprofen and Voltaren, as in addition to being analgesics and relieving the pain, they also target the inflammation which can help speed up the process of recovery.
Corticosteroid injections: if the pain is severe, your doctor may suggest injections of corticosteroids into your foot, this is usually done under local anesthesia, however, it is important to note that corticosteroid injections are usually used as a primary line of treatment only for severe cases, or otherwise reserved as an advance treatment for those who do not improve after a couple of months of applying conservative treatments, this is due to the possible negative side effects of corticosteroid injection including fat pad atrophy and rupture of the plantar fascia.
Orthotics: shoe inserts are important in the management of heel spur symptoms, as they can decrease the magnitude of the weight-bearing load on the heel, they can do so by increasing the height of the shoes which provides more cushioning between the heel and the ground. It was also found that softer and thicker appropriately sized orthotics can decrease the weight load on the calcaneus bone even further, which helps to greatly reduce the pain associated with heel spurs. (8)
A clinical study indicated that 10/16 of its participants who suffered from calcaneal spurs have reported a 70-100% decrease in their pain after using thick orthotics increasing the heel height and reducing the impact during weight-bearing daily activities. (9)
Orthotics also can play a significant role in treating plantar fasciitis that often coexists with heel spurs, a systematic review study of 19 clinical trials that included 1660 participants, reported that foot orthotics have been shown to reduce plantar heel pain in adults who have used them for a duration of (7-12) weeks. (10) Another clinical trial even found that orthotics can be noticeably better than the use of non-steroidal anti-inflammatory medications, heel cups, or corticosteroid injections. (11)
You can try either over-the-counter orthotics or get them custom-made to your foot size and shape. However, custom-made orthotics are usually expensive, ranging from 100-400 USD, and in real-life use, studies have shown that prefabricated OTC orthotics are usually as effective as the custom-made ones in treating heel pain.
That being said, using any OTC heel pad that is not designed for treating your foot condition will not produce great results as these heel pads are not made to provide structural support, and often just capable of mild shock absorption. Heel That Pain offers Heel Seats foot orthotics that use a unique and revolutionary technology called fascia-bar, which has been found, through a clinical trial conducted by the University of Iowa, to be 2 times more effective in relieving heel pain when compared to other leading orthotics brands. This is due to its amazing dense and soft Kraton cushion that has significant shock absorption ability, in addition to providing extensive support to both your heel and plantar fascia during weight-bearing activities, reducing the pain from plantar fasciitis and heel spurs, and accelerating your recovery, all with a very affordable cost.
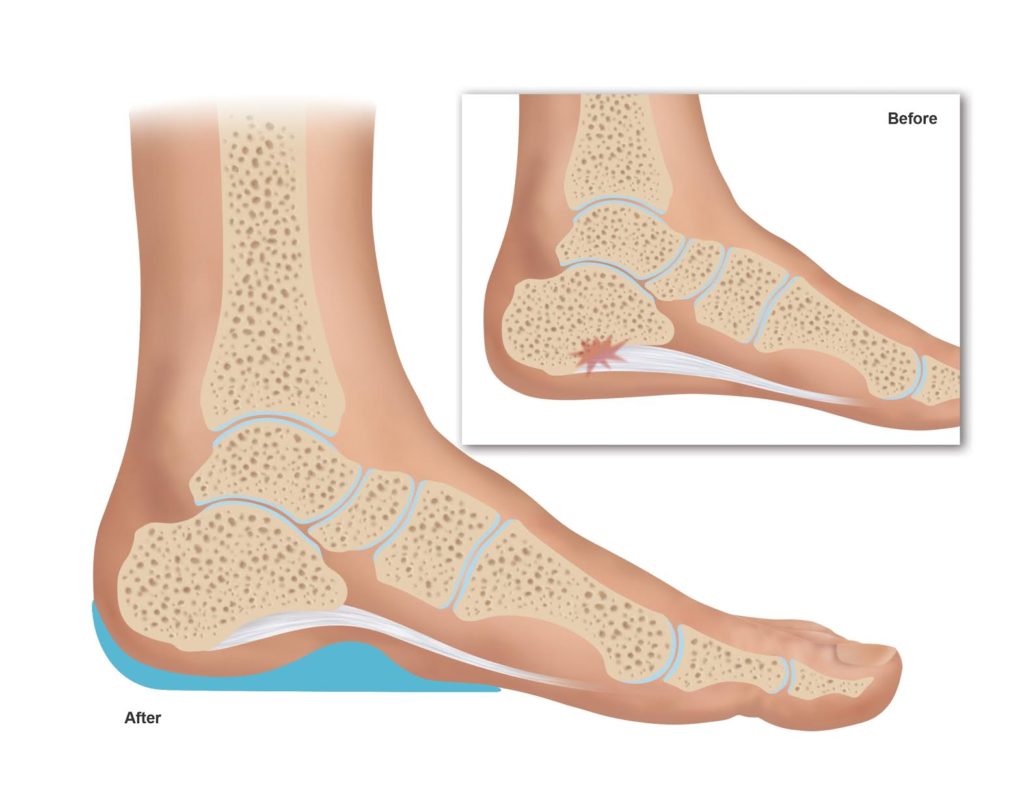
Another great well-designed product that is also offered by Heel That Pain is the Heel Seat Wraps, which are made to provide you with all the benefits of the Heel Seat shoe orthotics but with the ability to wear them barefoot, with sandals, slippers, or any kind of footwear. They are extremely supportive, soft on your feet, and flexible, with non-slip bottom that ensures your safety even when walking on slick floor or stairs. These heel wraps are great to maximize your treatment and speed up your recovery by wearing orthotics indoors and outdoors without putting on shoes at home.
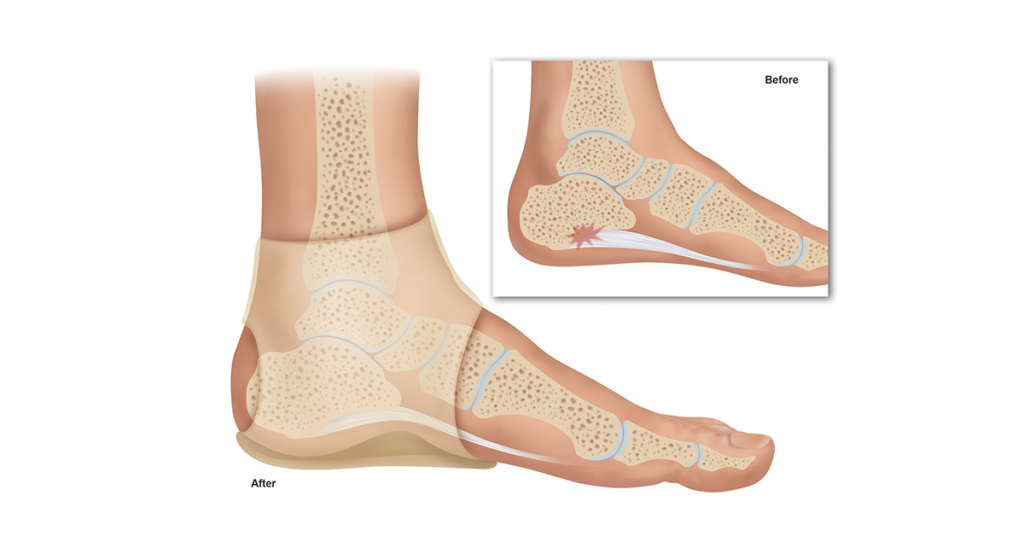
Stretching exercises: there are many stretching exercises that you can perform to warm up your plantar fascia, stretch the surrounding muscles and reduce the pain. These exercises include calf stretches, foot flexion, Achilles tendon, and plantar fascia stretches, they can be done with the help of a physical therapist or you can learn to do them yourself at home.
Strapping/ taping of the foot: athletic or kinesiology tape can be used to provide arch support and stabilize the structure of the foot. Try these taping methods to support your feet during activity.
Shoe change: high heels shoes, ill-fitted shoes or inappropriate ones can impact the way you bear your weight on your feet, contributing to the development of heel spurs, and if not corrected, this will aggravate your symptoms even further. Hence, it is necessary to pay attention to your footwear, ensuring that they are the accurate size, suitable for the activities you perform, and dense cushioning to provide shock absorption. If you are an active person who performs any form of high-impact exercise for long periods, changing your sports shoes every few months or replacing the insoles with shoe inserts can be necessary.
Advanced medical heel spur treatments including:
Botulinum toxin injection: this is occasionally used as an alternative for corticosteroid injections, particularly when heel spurs are accompanied by a plantar fasciitis diagnosis. This treatment has fewer side effects than corticosteroid injections, and it helps to reduce the pain associated with heel spurs and plantar fasciitis while improving overall foot functions.
Radiation therapy: ionizing radiation has an anti-inflammatory effect on various types of cells, several studies have reported its efficacy in treating the symptoms resulting from heel spurs, (12,13). One clinical trial has reported that the use of low doses of radiotherapy resulted in great pain reduction that persisted for years, with no signs of acute or late toxicity as a result of using the radiation therapy, suggesting that this is a cheap, simple, and safe technique to apply in the treatment of heel spurs. (14)
Iontophoresis and phonophoresis: these procedures are used to help a topical medication, corticosteroid in this case, deep into the soft tissues. Iontophoresis uses ionic forces (electric current) to deliver the medicine, while phonophoresis uses the thermal effect produced by ultrasound waves. Both procedures are similarly effective and greatly reduce the symptoms associated with both plantar fasciitis and heel spurs. However, these treatments are required to be done 2 to 3 times per week, which makes them less practical and cost-effective for regular people, hence they are often prescribed in the process of treating athletes who have the need and resources to do so.
Ultrasound therapy: using certain doses of ultrasound has a therapeutic and analgesic effect in treating heel spurs’ pain. It was found that the dose of 0.8 W/cm2 was capable of reducing pain by 34% after 5 sessions, by 50% after 10 sessions, and by 71% 4 weeks after the completion of therapy. However, this treatment requires multiple sessions per week so it can be time-consuming.
Extracorporeal shock-wave therapy (ESWT): this is a non-invasive treatment utilizing the delivery of high-pressure shock waves to the soft tissues in the affected area, significantly reducing pain and inflammation. This is thought to be due to its ability to stimulate the blood flow which increases the immune response and the healing process, additionally, it can shut down the pain neuronal pathways in the affected area, and help in the regeneration of the healthy tissues. A study investigating the effectiveness of ESWT in treating heel spurs has reported that after administering one session weekly for 5 weeks, 66.7% of all participants have reported excellent results with no more painful experiences, while the pain was reduced by 50% in 15.7% of the cases, and only 17.6% of participants had no satisfactory results. (15)
Another study compared the effectiveness of ESWT to ultrasound therapy in treating heel spurs symptoms, the study concluded that while both techniques significantly reduce pain, much fewer ESWT sessions were needed to produce the same results as ultrasound, which suggests that ESWT is more effective than ultrasound therapy. (16)
Surgery: this is reserved as a last option of treatment if all other conservative treatments have failed after following for 6 months to a year, and the less invasive procedures have also been considered without success. There are various approaches of surgery that are used in the treatment of heel spurs, they involve either removal of the spur only, focus on the release of the plantar fascia without the removal of the spur, or removing the spur and releasing the fascia at the same time. The surgery often has a high success rate, however, all surgeries come with possible short and long-term complications that should be taken into account before considering this option. More advanced techniques have been developed in recent years to minimize the recovery time from the surgery and the possible side effects, including endoscopic plantar fasciotomy and percutaneous release of the plantar fascia.
Addressing heel spur myths
Many myths surround the topic of heels spurs, therefore, it is important to educate yourself about this condition and be able to separate facts from fiction.
Can heel spurs break through the foot skin?
The answer to this question is no, it is a myth that heel spurs can get so long that they can penetrate the skin, and although they can get sometimes to a point where they can be felt or become visible underneath the foot, they can’t pierce through the skin.
Can you dissolve a heel spur?
Well, the answer to this question is unclear as there is no scientific evidence that supports this theory, and despite heel bone spurs being a build-up of calcium deposits, no exact substance or vitamin has been shown with certainty to dissolve these bone protrusions. Hence, it is important to stick to evidence-based science when it comes to the prevention and treatment of heel spurs.
How do you break a heel spur?
As mentioned earlier, heel spurs can be removed surgically by a medically trained specialist, so please do not attempt to break your heel spurs a this can be very dangerous and have serious complications. Heel spurs can rarely break on their own though, they then get lodged into the surrounding soft tissue, which can lead to an increase in the intensity of symptoms.
Can heel spurs cause back or hip pain?
Back pain or hip pain is not typical symptoms of heel spurs; however, some indirect correlation can exist as a result of long-term untreated heel spurs that can then impact the way the person carries their weight on their feet, leading to a change in their gait, putting more pressure on certain parts or joints in their body to compensate for the person’s inability to put on all their body weight on their struggling foot, this will consequently lead to pain in their lower back or hip joints.
What is the prognosis of heel bone spurs?
Although heel spurs can cause a lot of pain and discomfort when they are symptomatic, 80% to 90% of cases will greatly improve or completely recover from the symptoms, through following conservative treatments. The improvement can happen within a few weeks to months; hence it is important to stick properly to the conservative treatment and allow your feet time to heel. For those who do not improve or get worse after following the conservative and treatment for 6 months to a year, surgery may be needed to relieve the symptoms and restore the full function of the foot.
How to prevent heel spurs
- Maintain a healthy weight.
- Wear appropriate shoes for the activity you are performing.
- Ensure your shoes is well-fitted and that they have great heel and arch support using dense and soft materials to cushion the bottom of your feet and provide shock absorption and structural support.
- Try to avoid intense prolonged high-impact activities.
- Always take breaks when standing for too long to alleviate the vertical pressure on your feet.
- If you experience any pain in the bottom of your feet, stop doing the activity immediately and rest, as pushing through the pain will only aid in the developing or worsening of any heel condition.
References
- Beytemür, O., & Öncü, M. (2018). The age dependent change in the incidence of calcaneal spur. Acta orthopaedica et traumatologica turcica, 52(5), 367–371. https://doi.org/10.1016/j.aott.2018.06.013
- Bergmann J. N. (1990). History and mechanical control of heel spur pain. Clinics in podiatric medicine and surgery, 7(2), 243–259.
- Weiss E. (2012). Calcaneal spurs: examining etiology using prehistoric skeletal remains to understand present day heel pain. Foot (Edinburgh, Scotland), 22(3), 125–129. https://doi.org/10.1016/j.foot.2012.04.003
- Menz, H. B., Zammit, G. V., Landorf, K. B., & Munteanu, S. E. (2008). Plantar calcaneal spurs in older people: longitudinal traction or vertical compression?. Journal of foot and ankle research, 1(1), 7. https://doi.org/10.1186/1757-1146-1-7
- Li, J., & Muehleman, C. (2007). Anatomic relationship of heel spur to surrounding soft tissues: greater variability than previously reported. Clinical anatomy (New York, N.Y.), 20(8), 950–955. https://doi.org/10.1002/ca.20548
- Moroney, P. J., O’Neill, B. J., Khan-Bhambro, K., O’Flanagan, S. J., Keogh, P., & Kenny, P. J. (2014). The conundrum of calcaneal spurs: do they matter?. Foot & ankle specialist, 7(2), 95–101. https://doi.org/10.1177/1938640013516792
- Toumi, H., Davies, R., Mazor, M., Coursier, R., Best, T. M., Jennane, R., & Lespessailles, E. (2014). Changes in prevalence of calcaneal spurs in men & women: a random population from a trauma clinic. BMC musculoskeletal disorders, 15, 87. https://doi.org/10.1186/1471-2474-15-87
- Goske, S., Erdemir, A., Petre, M., Budhabhatti, S., & Cavanagh, P. R. (2006). Reduction of plantar heel pressures: Insole design using finite element analysis. Journal of biomechanics, 39(13), 2363–2370. https://doi.org/10.1016/j.jbiomech.2005.08.006
- Wibowo, D. B., Harahap, R., Widodo, A., Haryadi, G. D., & Ariyanto, M. (2017). The effectiveness of raising the heel height of shoes to reduce heel pain in patients with calcaneal spurs. Journal of physical therapy science, 29(12), 2068–2074. https://doi.org/10.1589/jpts.29.2068
- Whittaker GA, Munteanu SE, Menz HB, Tan JM, Rabusin CL, Landorf KB. (2017). Foot orthoses for plantar heel pain: a systematic review and meta-analysis. Br J Sports Med. [Medline].
- Lynch DM, Goforth WP, Martin JE, Odom RD, Preece CK, Kotter MW. (1998). Conservative treatment of plantar fasciitis. A prospective study. J Am Podiatr Med Assoc, 88:375–80.
- Schneider, O., Stückle, C. A., Bosch, E., Gott, C., & Adamietz, I. A. (2004). Effectiveness and prognostic factors of radiotherapy for painful plantar heel spurs. Strahlentherapie und Onkologie : Organ der Deutschen Rontgengesellschaft … [et al], 180(8), 502–509. https://doi.org/10.1007/s00066-004-1204-7
- Seegenschmiedt, M. H., Keilholz, L., Stecken, A., Katalinic, A., & Sauer, R. (1996). Radiotherapie beim plantaren Fersensporn. Indikation, Technik, klinische Ergebnisse bei unterschiedlichen Dosiskonzepten [Radiotherapy of plantar heel spurs: indications, technique, clinical results at different dose concepts]. Strahlentherapie und Onkologie : Organ der Deutschen Rontgengesellschaft … [et al], 172(7), 376–383.
- Kędzierawski, P., Stando, R., & Macek, P. (2017). Retrospective evaluation of the effectiveness of radiotherapy in patients with plantar fascitis (heel spurs). Reports of practical oncology and radiotherapy : journal of Greatpoland Cancer Center in Poznan and Polish Society of Radiation Oncology, 22(3), 209–211. https://doi.org/10.1016/j.rpor.2016.11.001
- Yalcin, E., Keskin Akca, A., Selcuk, B., Kurtaran, A., & Akyuz, M. (2012). Effects of extracorporal shock wave therapy on symptomatic heel spurs: a correlation between clinical outcome and radiologic changes. Rheumatology international, 32(2), 343–347. https://doi.org/10.1007/s00296-010-1622-z
- Krukowska, J., Wrona, J., Sienkiewicz, M., & Czernicki, J. (2016). A comparative analysis of analgesic efficacy of ultrasound and shock wave therapy in the treatment of patients with inflammation of the attachment of the plantar fascia in the course of calcaneal spurs. Archives of orthopaedic and trauma surgery, 136(9), 1289–1296. https://doi.org/10.1007/s00402-016-2503-z
Further Reading on Heel Spurs
| Heel Spurs vs. Plantar Fasciitis | Heel Spur Facts | Bone Spur Treatments |
| Heel Spur Myths | Heel Spur Causes | Heel Spur Exercises |


